ENDOSCOPIC APPROACH FOR RESECTION OF A SMALL FRONTAL RECESS OSTEOMA CAUSING HEADACHE
Summary
Paranasal sinus osteomas are common, slow-growing, benign tumors that are usually asymptomatic. Most of these neoplasms are detected incidentally during routine radiological investigation of unrelated complaints. Symptoms and complications tend to develop when the mass expands; however, even a small osteoma in the frontal recess can interfere with aeration of the frontal sinus and lead to headache. A 34-year-old woman presented to our clinic with headache affecting the fronto-ethmoidal region. The Waters view and computerized paranasal sinus tomography showed an osteoma in the right frontal recess and a middle concha bullosa on the left side. There were no abnormalities on neurological and ophthalmologic examination. Other causes of headache were excluded and the frontal recess osteoma was treated endoscopically for the relieving of the chronic frontal headache.Introduction
The osteomas are frequently seen benign tumors of paranasal sinuses.[1,2] These tumors are usually asymptomatic and detected incidentally during the radiological investigation. They can be symptomatic depending on their location, size, rate of growth and expansion.[3] The treatment for paranasal sinus osteoma is surgical excision; however, all osteomas do not require surgery. For many years, osteomas were treated with open surgical approaches like as the osteoplastic flap technique, lateral rhinotomy, and direct anterior surgical exposure of the frontal sinus. Nowadays, many forms of nasal and paranasal pathology including osteomas may be treated by endoscopic methods. The indications for surgery and the optimal approach are matters of controversy. In this article, we describe a patient who had a small osteoma in the frontal recess that was treated endoscopically.Case Presentation
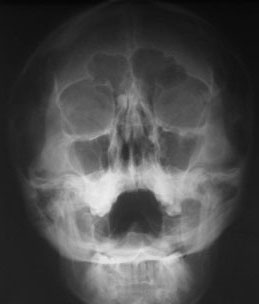
In December 2001, a 34-year-old woman was seen at the Ear, Nose, and Throat Department of our center with the complaints of headache affecting the fronto-ethmoidal region, nasal obstruction, and postnasal discharge. She had had the headache problem for approximately 2-3 years. There were no abnormalities on neurological and ophthalmologic examination. Otorhinolaryngological examination revealed a nasal hump, septal deviation, and mucopurulent discharge. Plain radiography with a Waters view showed a small osteoma in the right fronto-ethmoidal region (Figure 1). The patient was treated with a 14-day course of oral antibiotics and systemic decongestant.One month later, the postnasal discharge had decreased but the headache and nasal obstruction remained unchanged. Another Waters view x-ray was obtained and coronal paranasal computed tomography (CT) was performed. CT showed a dense, well-circumscribed mass measuring 9x8x6 mm in the right frontal recess, and a middle concha bullosa on the left side (Figures 2). The concha bullosa was not in contact with the nasal septum or the lateral nasal wall.
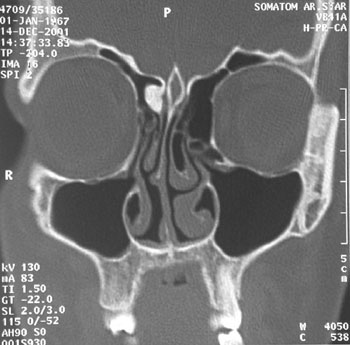 | Computed tomography scanning in the coronal plane demonstrated the osteoma in the right frontal recess |
The patient underwent endoscopic sinus surgery (ESS) to treat the concha bullosa and osteoma, and septorhinoplasty was performed to reconstruct the nasal-endonasal deformity. During ESS, the rigth middle concha was mobilized medially and the frontal recess was exposed via an uncinatectomy. Both 0-degree and 30-degree endoscopes were used during the procedure. This allowed sufficient visualization of the surgical field and facilitated manipulation of the osteoma. The tumor was partially obstructing the frontal recess, and the mucosa around the mass appeared normal. Care was taken to avoid traumatizing the surrounding mucosa; thus, normal physiology was preserved and it was not necessary to obliterate the frontal sinus. The osteoma was mobilized and extracted using a Freer elevator. No drilling was necessary. There was a small amount of hemorrhage, but this was easily controlled.
The patients pain disappeared completely in the first postoperative week. In light of this, we attributed her fronto-ethmoid headache to the osteoma. The findings on follow-up CT at 6 months are shown in Figure 3. At 12 months post-surgery, she remained free of symptoms. Nasal endoscopic examination at this stage revealed no evidence of inflammation or adhesions, and showed normal epithelialization of the right frontal recess.
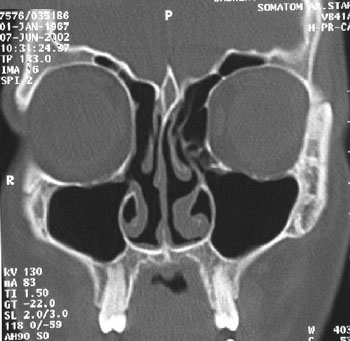 | Computed tomography scanning in the coronal plane at 6 months post-surgery revealed a patent frontal recess, no residual tumor in the recess, and normal aeration of the frontal sinus |
Discussion
Paranasal sinus osteomas are slow-growing, encapsulated, benign tumors that are most often found in the frontal and ethmoid sinuses, and less frequently in the maxillary and sphenoid sinuses.[1,2] Most of these tumors are asymptomatic, and are detected during routine radiological investigation of unrelated complaints. Depending on location, size, and rate of growth, expansion of the mass may produce a variety of symptoms and complications.[3] The tumor may cause cosmetic deformity directly, or may obstruct sinus ostia and lead to sinusitis or mucocele formation.[4,5,6,7] If the neoplasm extends beyond the sinus boundary and begins to erode bone, vital anatomic structures such as the orbit and the cranium can be affected, producing a range of symptoms and problems. Orbital extension can displace the eyeball, impair extraocular muscle motility, and cause diplopia, proptosis, exophthalmus, optic nerve compression, papillary atrophy, and impaired vision.[1,3,4,5,6,8,9] Intracranial extension from the frontal, ethmoid, and sphenoid sinuses may lead to cerebrospinal fluid (CSF) leakage, intracranial infection, or abscess.[6,7]The frontal recess is an hourglass-shaped space that is defined by its surrounding structures, namely, the middle turbinate, uncinate process, lamina papyracea, ethmoid bulla, and agger nasi cells.[10] Obstruction of this recess results in insufficient ventilation of the frontal sinus. When the drainage route for this cavity is blocked, the entrapped oxygen is absorbed by the mucosa and causes negative pressure within the sinus, which produces pain.[11] A small osteoma in the frontal recess can affect the patency of the frontal recess, decrease frontal sinus aeration, and produce negative pressure and headache.[11] Headache may also be the direct result of pressure from enlargement of the osteoma. Further, enlargement of small osteomas, especially those in specific locations such as the frontal recess and ethmoidal cells, may cause headache because these cavities cannot expand to any significant degree.
The management of frontal sinus and recess osteoma remains controversial. The only suspected pathology for headache must be the osteoma and all possible causes like as intracranial orbital and other paranasal pathologies must be excluded in the preoperative evaluation of the headache.
For decades, osteomas of these regions were treated with open surgical approaches. External approaches, including the osteoplastic flap technique, lateral rhinotomy, and direct anterior surgical exposure of the frontal sinus, have been used to access large osteomas of the fronto-ethmoidal region, with or without involvement of surrounding structures.[9,12]
Today, endoscopic methods are used to treat many forms of nasal and paranasal pathology, including chronic or complicated sinusitis, dacryocystitis, orbital decompression, optic nerve decompression, cerebrospinal fistula, some tumors of the nasal and paranasal sinuses, and choanal atresia. Patient selection for ESS is important in cases of paranasal sinus osteoma. For example, not all fronto-ethmoid osteomas can be removed this way. Small frontal sinus osteomas that are located medial to the sagittal plane of the lamina papyracea and based in the postero-inferior wall of the sinus can be excised by ESS, as can most ethmoid sinus and frontal recess osteomas.[6]
In ESS, the following steps are used to expose the frontal recess[16,17]:
- The middle turbinate is mobilized medially.
- The antero-superior aspect of the uncinate process is completely removed.
- The antero-superior attachment of the bulla ethmoidalis can be removed to better visualize the recess.
- If the anterior frontal and agger nasi cells are obstructing fronto-nasal outflow and blocking the surgeons view of the frontal recess, these should be removed, taking care to preserve the mucosa of the frontal recess and ostium.
Conclusion
In appropriate osteoma cases, the endoscopic approach offers a high probability of recovery with low risk of morbidity. Any patient with a small osteoma who has chronic headache should be reviewed. If other causes are excluded, then the tumor can be removed by ESS. Careful use of nasoendoscopic technique can prevent CSF leakage and cosmetic deformity, which are relatively high risks with the osteoplastic flap technique. Also, when endoscopic surgery is used for the removing small osteomas suspected to be causing headache, unnecessary followup of osteoma with frequent radiographs can be avoided.Reference
1) Koivunen P, Lopponen H, Fors AP, Jokinen K. The growth rate of osteomas of the paranasal sinuses. Clin Otolaryngol 22(2): 111-4, 1997. [ Özet ]
2) Earwaker J. Paranasal sinus osteomas: a review of 46 cases. Skeletal Radiol 22(6): 417-23, 1993. [ Özet ]
3) Atallah N, Jay MM. Osteomas of the paranasal sinuses. J Laryngol Otol 95(3): 291-304, 1981. [ Özet ]
4) Ataman M, Ayas K, Gursel B. Giant osteoma of the frontal sinus. Rhinology 31(4): 185-7, 1993. [ Özet ]
5) Onerci M, Hosal S, Korkmaz H. Nasal osteoma: a case report. J Oral Maxillofac Surg 51(4): 423-5, 1993. [ Özet ]
6) Schick B, Steigerwald C, el Rahman el Tahan A, Draf W. The role of endonasal surgery in the management of frontoethmoidal osteomas. Rhinology 39(2): 66-70, 2001. [ Özet ]
7) Koyuncu M, Belet U, Sesen T, Tanyeri Y, Simsek M. Huge osteoma of the frontoethmoidal sinus with secondary brain abscess. Auris Nasus Larynx 27(3): 285-7, 2000. [ Özet ]
8) Hehar SS, Jones NS. Fronto-ethmoid osteoma: the place of surgery. J Laryngol Otol 111(4): 372-5, 1997. [ Özet ]
9) Schwartz MS, Crockett DM. Management of a large frontoethmoid osteoma with sinus cranialization and cranial bone graft reconstruction. Int J Pediatr Otorhinolaryngol 20(1): 63-72, 1990. [ Özet ]
10) Stammberger H. Functional endoscopic sinus surgery. St. Louis: BC Decker, 1991: 82-87.
11) Leiberman A, Tovi F. A small osteoma of the frontal sinus causing headaches. J Laryngol Otol 98(11): 1147-9, 1984. [ Özet ]
12) Savic DL, Djeric DR. Indications for the surgical treatment of osteomas of the frontal and ethmoid sinuses. Clin Otolaryngol 15(5): 397-404, 1990. [ Özet ]
13) Huang HM, Liu CH, Lin KN, Chen HAT. Giant ethmoid osteoma with orbital extension, a nasendoscopic approach using an intranasal drill. Laryngoscope 111:430-432, 2001. [ Özet ]
14) Schenck NL: Frontal sinus disease III. Experimental and clinical factors in failure of the frontal osteoplastic operation. Laryngoscope 85(1): 76-92, 1975. [ Özet ]
15) Akmansu H, Eryilmaz A, Dagli M, Korkmaz H. Endoscopic removal of paranasal sinus osteoma: A case report. J Oral Maxillofac Surg 60: 230-232, 2002. [ Özet ]
16) Terrell JE. Primary sinus surgery. In Cummings CW, ed: Otolaryngology Head & Neck Surgery, 3rd ed. Philadelphia: Mosby, 1998: 1156-1157.
17) Weber R, Draf W, Kratzsch B, Hosemann W, Schaefer SD. Modern concepts of frontal sinus surgery. Laryngoscope 111:137-146, 2001. [ Özet ]