IMPACT OF MICRODEBRIDER IN SURGICAL TREATMENT OF NASAL POLYPOSIS IN TERMS OF HEALTH RELATED QUALITY OF LIFE AND OBJECTIVE FINDINGS: A COMPERATIVE RANDOMIZED SINGLE BLINDED CLINICAL STUDY
Summary
Background: A prospective randomized single-blinded clinical study to compare the outcomes of a total of 97 patients in two groups with nasal polyposis treated surgically with traditional instruments and powered instruments.Methods: Prospective randomized single-blinded clinical study in a tertiary care center with 97 patients evaluated in two groups undergoing endoscopic sinus surgery for nasal polyposis. Medical Outcomes Study Short Form (SF-36)-general health status survey was used for quality of life assessment and Lund-Mackay radiologic and endoscopic scoring and acoustic rhinometric nasal volume measurements were used for objective evaluation between randomly allocated study and control groups in a single-blinded manner. The comparison was performed between the results preoperatively and 6-months postoperatively. Paired-t test was used for comparison of preoperative and postoperative results in each group. ANOVA test was used for inter-groups differences.
Results: Endoscopic, tomographic and acoustic rhinometric findings and self reported health status survey scores were improved postoperatively in both groups. However, there was an exception in radiologic scores for the forceps group; there was not any statistically significant difference between the preoperative and postoperative radiologic scores for both sides. When two groups were compared postoperatively there was no statistically significant difference. Both techniques showed no major complications.
Conclusion: Emphasizing on the identical results with objective and subjective outcomes measures between through cutting traditional instruments and microdebrider, this study stands as complementary to the previous papers stating satisfactory outcomes, minimal morbidities and improved surgeon and patient comfort with powered instruments in the treatment of nasal polyposis.
Introduction
Nasal polyps are intranasal structures that arise from the edematous nasal mucosa and extend through nasal cavity and paranasal sinuses. Their treatment depends both on surgical and medical managements. Since 1980's they have been surgically managed with impressive outcomes by Messerklinger's traditional instrumentation technique. The aim of this technique is to remove the pathologic tissues inside the ostiomeatal complex and to restore the corrupted mucociliary clearance and sinus ventilation without harming normal nasal physiology and anatomy [1-3]. Diffuse pathological tissues can be removed under clear vision by surgical intervention with less morbidity and minimal incisions.As in all operative procedures, surgeons continue to adopt and modify their techniques in order to achieve improved outcomes with fewer complications. One modification of the Functional Endoscopic Sinus Surgery technique which has become popular in recent years is the application of the microdebrider, a powered instrument designed to exenterate disease with decreased trauma to normal tissues. In 1994, Setliff and Parsons introduced microdebrider (shaver) to endoscopic sinus surgery [1]. This method provides satisfactory results by making dissection faster, almost bloodless and safe, and lets rapid healing of tissues without harming normal mucosa. Those powered instruments achieve a good surgical field by shaving and removing the soft tissues along with fluid and allow the intact mucosa to be protected during dissection [4,5]. There is also a possibility of getting biopsy specimens during surgery for histopathologic examination [5,7].
The description of a new technique provokes the question of whether that new technique provides a significant advantage in methodology over the conventional procedure. Previous studies about this subject focused on less tissue damage, less bleeding and complications [2-5]. This is the first clinical study using control and study groups simultaneously which was designed in a randomized single- blinded manner.
Measures of a patient's general health-status and functional well-being are essential for outcomes research because the response to treatment and the need for subsequent medical care are in large measure based on the patient's baseline functional level and well being.
The Medical Outcomes Study Short Form-36 (SF-36) is a valid and widely used general health status measure that contains 36 items measuring function in eight domains: physical functioning, role physical, bodily pain, general health, vitality, social functioning, role emotional and mental health. Scores for each domain can range from 0 to 100, with 100 representing perfect health. Normative values are available for the general population and for rhinosinusitis patients. Because the SF-36 has already been validated, is so widely accepted, and has normative values for the rhinosinusitis population, the Task Force on Rhinosinusitis recommends its use as the general health status instruments [8]. Recently SF-36 has already been used in many clinical studies, but this is the first study about its application in powered instrumentation in the treatment of nasal polyposis.
The description of a new technique provokes the question of whether that new technique provides a significant advantage in methodology over the conventional procedure. The present study was designed to evaluate the use of microdebrider as compared to standard functional endoscopic sinus surgical techniques. For dealing with this matter we used general health status instrument SF-36 as a subjective parameter and endoscopic and tomographic scoring as objective parameters in a prospective, randomized and single-blinded manner.
Methods
Patients:Subjects of the present study were 167 patients who were treated with FESS for nasal polyposis in our clinic between January, 2002 and January, 2005. Ninety-seven of these patients completed the postoperative follow-up were included in the present prospective series. All patients had been given two-weeks of systemic (1 mg/kg prednisolon p.o. for one week and tapered in the following week) and topical steroids (Budesonide two times daily; 2x2 puff for each nostril which means 400 mcg total daily dose and 1 puff consists of 50 mcg budesonide) before surgery. Lifelong topical steroids prescribed for each patient in the postoperative period. No boosters of systemic steroids were given during the first 6-months postoperative period, at the end of which the objective and subjective evaluation were performed. Informed consent was obtained from patients and permission was taken from the local ethic comity. The subjects were randomly selected for treatment (microdebrider) and control (traditional instruments) groups, and single-blinded technique was used. A neutral party kept the code as to who's who and disclosed it only at the end of data gathering. One of the junior authors (Lale O, MD) performed the objective and subjective outcomes measures without knowing to which group the patient belongs.
Exclusion criteria:
The patients having systemic and local disorders that might effect patient's quality of life seriously except for nasal polyposis and allergic rhinitis were excluded from both study and control groups. Uncontrolled arterial hypertension and diabetes, lung, kidney and liver disorders, neurologic and psyciatric conditions, locomotor system disorders, asthma, Cartegener syndrome and cystic fibrosis are among these disorders. Also revision cases and pediatric population was not included in both groups.
Surgery:
In this study, 97 consecutive nasal polyposis patients from our practice formed the sample. Of these patients, 46 were operated on by using the microdebrider (Unidrive II, Karl-Storz, Tutlingen, Germany), and 51 by standard technique using through cutting instruments as described by Kennedy. In the microdebrider group, the entire procedure was completed using microdebrider device, including the sphenoethmoidectomy, frontal recess exploration, and maxillary antrostomy, depending on the nature of the patient's disease process. The use of forceps during the procedure in this group was minimal. All of the operations were performed under strict supervision of senior author (Samim E, MD) in order to achieve standardization.
Evaluation of Quality of Life:
Patients were asked to complete self-assessment surveys to have information about their physical and mental functioning both preoperatively and 6-months postoperatively on an objective basis. This was managed by “The Medical Outcomes Study Short Form-36 (SF-36)-general health status instrument”. It is widely accepted by other medical disciplines and proposed by the Task Force on Rhinosinusitis (15) .The scores were calculated and interpreted by the free website www.sf-36.org/demos/SF-36.html. In our study we used PCS (physical comment summary) and MCS (mental comment summary) that represent mean values for physical and mental health status instead of separate scores for 8 distinct areas. The scores were given according to a 0-100 scale.
Assessment of objective parameters
Tomographic and Endoscopic Data:
Both groups of patients were staged preoperatively and postoperatively according to the Lund-Mackay staging system, recommended by the Task Force on Rhinosinusitis of the American Academy of Otolaryngology-Head and Neck Surgery. They were scored by postoperative endoscopic follow-up findings and preoperative and postoperative CT findings [8].
The scoring system that is developed for the sinus groups is based upon the tomographic appearances. Every sinus group is scored according to a numerical pattern: 0=no anomaly, 1=partial opacification, 2=complete opacification.
The endoscopic appearances of the nasal cavities are also scored according to the existence of the polyps (0=no polyps, 1=polyps confined to middle meatus, 2=polyps exceeding middle meatus), existence of the secretions (0=no secretion, 1=clear and thin, 2=thick, mucoid, suppurative), edema, scarring or synechia and crusting (for every one (0=none, 1=mild, 2=serious). Those appearances are evaluated in regular postoperative visits, but are not included in the staging system [8]. The scores at 6-months postoperatively were taken into acount in this study.
Acoustic Rhinometric data
All patients' acoustic rhinometric measurements were obtained preoperatively and 6-months postoperatively while decongested and non-decongested and then total nasal volumes were calculated and recorded.
Data Analysis
Data forms were edited, coded, and entered into a computed data base. SPSS/PC+ statistical software were used to facilitate data analysis. We used paired-t test for comparing pre and postoperative results in a definite group and ANOVA test for inter-groups comparison. If the probability of the observed difference was less than 0.05, the difference was statistically significant.
Results
Demographic data:Ninety-seven patients with nasal polyposis evaluated in two groups were included in the study. Of the 51 patients constituting the traditional instrument group, 18 were female (35,3%) and 33 were male (64,7%) (Age range 17-71 years; mean age 43,39 years). Alternatively, of the 46 patients constituting the powered instrument group, 15 were female (32,6%) and 31 were male (63,4%) (Age range 16-70; mean age 48,24) .
Evaluation of quality of life:
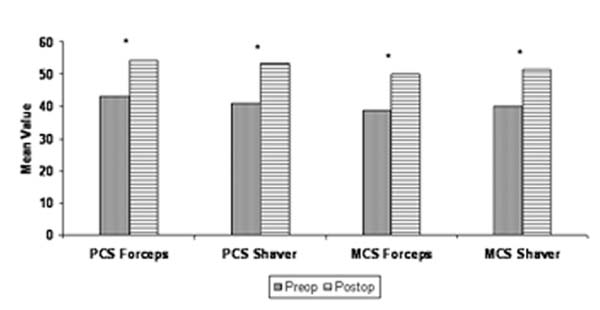
Health status scores were calculated in two forms: Physical comment summary (PCS) and mental comment summary (MCS). When the preoperative and postoperative scores were compared by paired-t test, both groups showed statistically significant difference (p<0,05). When the postoperative values for each group were compared by one way ANOVA test, there was no statistically significant difference (p>0,05). The results were summarized in graphic 1.
 Büyütmek İçin Tıklayın |
Graph 1: Showing the results of evaluation of guality of life in and between two groups. *: There was statistically significant difference in these comparisons made in by paried t-test |
Radiographic and endoscopic improvement
When the preoperative and postoperative scores were compared by paired-t test only the microdebrider group showed statistically significant difference (p<0,05) for both nasal cavity. When the postoperative scores for each group were compared by one-way ANOVA test they showed no statistically significant difference. The results were summarized in graphic 2.
 Büyütmek İçin Tıklayın |
Graph 2: Showing the results of tomographic assessment. *: There was statistically significant difference in these comparisons made in by pariedt-test |
Postoperative endoscopic follow-up scores were as follows:
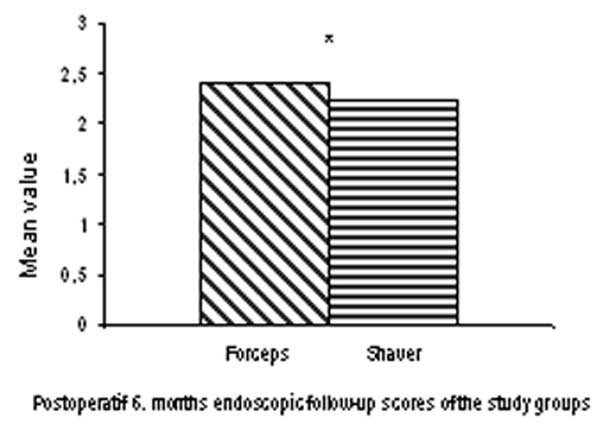
Postoperative 6th month scores were 2,39+/-2,06 for the forceps group and 2,24+/-2,72 for the shaver group. When the scores for each group were compared by one-way ANOVA test they showed no statistically significant difference. The results were summarized in graphic 3.
 Büyütmek İçin Tıklayın |
Graph 3: Showingthe results postoparhive endoscopicis assessment. *: There was statistically no significant difference in these comparisons made in by ANOV A test |
Nasal Volume improvement
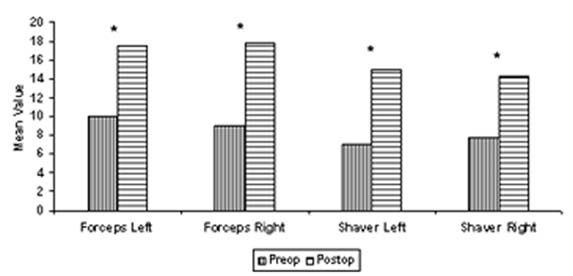
Total nasal volume values were calculated by acoustic rhinometry system. When preoperative and postoperative values were compared for the forceps group with and without decongestion with paired-t test, there was statistically significant difference (p<0,05). There was also statistically significant difference for the shaver group. When the postoperative values of each group were compared by one-way ANOVA test, there was also no statistically significant difference. The results were summarized in graphic 4.
 Büyütmek İçin Tıklayın |
Graph 4: Showing the results of a coustic rhinometric findings *: There was statistically significant difference in these comparisons made in by paried t-test |
Discussion
Since Kennedy's description of functional endoscopic sinus surgery (FESS) in 1985, this technique has become the method of choice in surgery for sinus disease. Surgeons soon recognized that very delicate and precise surgery was recommended by the functional approach. Standard instruments usually tear tissues and stripe mucous membranes. Consequently, this leads to increased bleeding with decreased visibility and undesirable frequency of complications and scarring. In 1994, Setliff [1] introduced powered shavers to sinus surgery. These instruments offered the distinct advantages of simultaneous suction and greatly increased cutting precision during endoscopic sinus surgery [2,3].The increased surgical precision can thus be expected to lead to improved functional results using the standard FESS technique and powered instrumentation. In the literature, there are several reports emphasizing significantly decreased blood loss, reduced synechia formation, a reduced ostial occlusion rate, and faster healing occurred in the shaver group. This article is actually the first report comparing the standard technique with through cutting forceps and powered instruments depending on both standardized subjective and objective outcomes measures in a randomized single-blinded manner.
In postoperative follow-up period, there is no special advice to have all patients' control tomograms routinely. The best period for the control tomogram is between 4th and 6th months. It is better to follow patients for 2 years [9]. In our study, all the objective and subjective outcomes measures were performed strictly at the 6-months postoperatively as well as high resolution paranasal sinus tomography [10]. Of course, postoperative follow-ups have been continued at least for two years but the results of these long term follow-ups are not mentioned here.
Lund and Kennedy claim that a staging system limited to the CT appearances is far from being optimal due to the interpretation problems related to previous surgery, naturally hypoplasic frontal sinus and interfered appearances of inflamed mucosa and thickened mucous. They also claim that the symptoms and disease progress have poor correlation. However, CT is a valuable objective diagnostic tool [11]. The aim of the staging systems used for patient follow-up is to evaluate the prognostic factors effecting the etiology and outcome of nasal polyposis, to classify patient groups evaluating radiological, endoscopic, operative and laboratory findings, to determine treatment modalities and to evaluate the outcomes of these treatment modalities while comparing to the outcomes of other authors. We made some modifications on the staging system proposed by Task Force on Rhinosinusitis of the American Academy of Otolaryngology-Head and Neck Surgery. They also stress on the importance of new studies on modifications and improvements on present systems and production of new staging systems having wide field of usage [9,12].
Metson stressed on the health status instruments as new tools to evaluate the efficiency of treatment. This information also helps health crew to inform patients about their disease and treatment alternatives. Therefore, disease specific health status instruments are important when determining the efficacy of the endoscopic sinus surgery. However, they are not adequate without general health status instruments. The SF-36 measures general patient functioning and helps determine the relative effects of the accompanying diseases. Further studies are essential to understand if there is a necessity to design new sinusitis specific health status instruments or not [8].
In our study, we found out the quality of life to improve statistically significant preoperatively versus postoperatively in both physical and mental health status in both groups of patients. But, when both groups were compared, there was no statistically significant difference. In the study design, our purpose was to change the subjective data of patients to objective data. According to our observations, in the shaver group, the subjective reports of the patients were better than those of the traditional group.
We believe that the statistically insignificant differences of the acoustic rhinometric and computed tomographic findings were due to the heterogenity of the patient groups and decreased measure sensitivity of the Lund-Mackay Staging System caused by its simplicity of interpretation.
The statistically insignificant difference between symptom scores of both groups is not entirely contradictory with the literature because the advantages attributed to the shaver is about the postoperative healing period and loss of long-term recurrences due to reduced synechia formation. Our symptom scale was filled in the postoperative 6th month and concerned with the last 2 months. Healing period is limited to 6 weeks even with the traditional technique.
The postoperative endoscopic appearance findings within both groups statistically were not significantly different. This finding is contradictory with the literature. But within the literature there are no signs of objective scoring system, so these comments are subjective. Our subjective comment about these patients is both groups are not different in terms of endoscopic appearance. Selivanova et al. claim that they have found the same postoperative findings as ours [13].
According to the statistical results, both groups of patients had benefit from surgery; both groups had improvements in quality of life, symptom frequency, endoscopic appearances, tomographic appearances, and acoustic rhinometry findings after surgery. However, according to these results, both groups are not superior to each other. This situation partially contradictory with the literature may be improved as our clinical experience with this device increases, and as our clinic has new models of this effective device. These findings may lead to better results in our further studies about this issue.
Conclusion
Emphasizing on the identical results with objective and subjective outcomes measures between through cutting traditional instruments and microdebrider, this study stands as complementary to the previous papers stating satisfactory outcomes, minimal morbidities and improved surgeon and patient comfort with powered instruments in the treatment of nasal polyposis.Reference
1) Setliff RC 3rd. The hummer: a remedy for apprehension in functional endoscopic sinus surgery. Otolaryngol Clin North Am 1996; 29(1): 95-104. [ Özet ].
2) Gross WE. Soft-tissue shavers in functional endoscopic sinus surgery (Standard technique). Otolaryngol Clin North Am 1997; 30(3):435-441. [ Özet ]
3) Christmas DA, Krouse JH. Powered instrumentation in functional endoscopic sinus surgery I: Surgical technique. Ear Nose Throat J 1996; 75(1): 33-6. [ Özet ]
4) Bernstein JM, Lebowitz RA, Jacobs JB. Initial report on postoperative healing after endoscopic sinus surgery with the microdebrider. Otolaryngol Head Neck Surg 1998; 118(6):800-3. [ Özet ]
5) Krouse JH, Christmas DA: Powered instrumentation in functional endoscopic sinus surgery. II: A comperative study. Ear Nose Throat J 1996; 75(1): 39-43. [ Özet ]
6) McGarry GW, Gana P, Adamson B. The Effect of microdebriders on tissue for histological diagnosis. Clinical Otolaryngology 1999; 22: 375-376. [ Özet ]
7) Zweig JL, Schaitkin BM, Fan CY, Barnes EL. Histopathology of tissue samples removed using the microdebrider technique: implications for endoscopic sinus surgery. Am J Rhinology 2000; 14(1): 27-32. [ Özet ]
8) Leopold D, Ferguson JB, Piccirillo JF. Outcomes assessment. Otolaryngol Head Neck Surg 1997; 117(3): 58-68. [ Özet ]
9) Rice DH. Endoscopic Sinus Surgery: Results at 2 -year follow-up. Otolaryngol Head Neck Surg 1989; 101: 476-9. [ Özet ]
10) Lund VJ, Kennedy DW. Staging for rhinosinusitis. Otolaryngology-Head and Neck Surgery 1997; 117: 35-40. [ Özet ]
11) Kennedy DW, Wright ED, Goldberg AN. Objective and subjective outcomes in surgery for chronic sinusitis. Laryngoscope 2000; 110(Suppl.94): 29-31. [ Özet ]
12) Metson RB, Glicklich RE. Clinical outcomes in patients with chronic sinusitis. Laryngoscope 2000; 110(Suppl.94): 24-28. [ Özet ]
13) Selivanova O, Kuehnemund M, Mann WJ, Amedee RG. Comparison of conventional instruments and mechanical debriders for surgery of patients with chronic sinusitis. Am J Rhinology 2003; 17(4): 197-202. [ Özet ]




